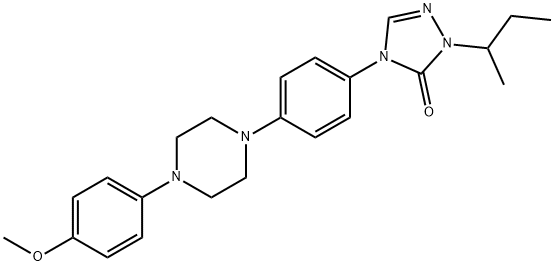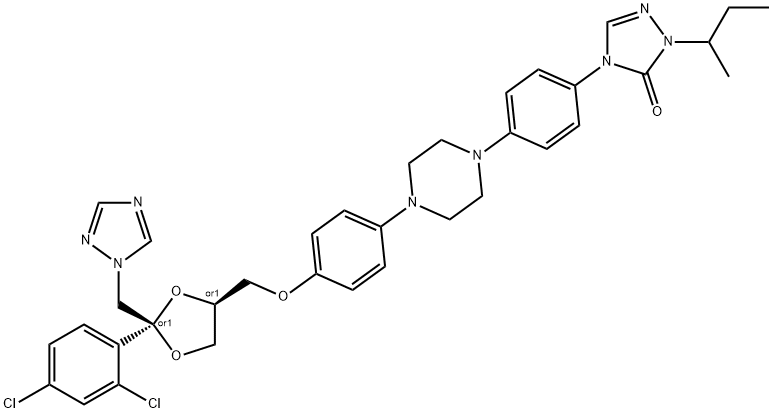
Itraconazole
- Product NameItraconazole
- CAS84625-61-6
- CBNumberCB4716071
- MFC35H38Cl2N8O4
- MW705.63
- EINECS617-596-9
- MDL NumberMFCD00870168
- MOL File84625-61-6.mol
- MSDS FileSDS
Chemical Properties
| Melting point | 166°C |
| Boiling point | 850.0±75.0 °C(Predicted) |
| alpha | -0.1~+0.1°(D/20℃)(c=10,CH2Cl2) |
| Density | 1.27 g/cm3 |
| Flash point | >110°(230°F) |
| storage temp. | 2-8°C |
| solubility | chloroform: 50 mg/mL, clear, colorless |
| pka | 3.7(at 25℃) |
| form | White powder |
| color | white |
| Water Solubility | Insoluble in water. Solube in chloroform at 50 mg/ml. Slightly soluble in ethanol or methanol |
| Merck | 14,5245 |
| Stability | Stable. Incompatible with strong oxidizing agents. |
| InChIKey | VHVPQPYKVGDNFY-UHFFFAOYSA-N |
| CAS DataBase Reference | 84625-61-6(CAS DataBase Reference) |
| EWG's Food Scores | 1 |
| NCI Dictionary of Cancer Terms | itraconazole |
| FDA UNII | 304NUG5GF4 |
| NCI Drug Dictionary | itraconazole |
| ATC code | J02AC02 |
Safety
| Symbol(GHS) |

|
|||||||||
| Signal word | Warning | |||||||||
| Hazard statements | H302-H315-H319-H335 | |||||||||
| Precautionary statements | P261-P264-P270-P301+P312-P302+P352-P305+P351+P338 | |||||||||
| Hazard Codes | Xi,Xn,T,F | |||||||||
| Risk Statements | 36/37/38-36/38-22-39/23/24/25-23/24/25-11 | |||||||||
| Safety Statements | 22-26-36-45-36/37-16 | |||||||||
| RIDADR | UN 3286 8(6.1)(3) / PGII | |||||||||
| WGK Germany | 3 | |||||||||
| RTECS | XZ5481000 | |||||||||
| HS Code | 2934990002 | |||||||||
| Hazardous Substances Data | 84625-61-6(Hazardous Substances Data) | |||||||||
| Toxicity | LD50 (14 day) in mice, rats, dogs (mg/kg): >320, >320, >200 orally (Van Cauteren) | |||||||||
| NFPA 704: |
|
Itraconazole Price
| Product number | Packaging | Price | Product description | Buy |
|---|---|---|---|---|
| Sigma-Aldrich I-015 | 1mL | $95.5 | Itraconazole solution 2.0?mg/mL (Methanol with 1% 1M HCl), ampule of 1?mL, certified reference material, Cerilliant? |
Buy |
| Sigma-Aldrich 419825 | 250mg | $208 | Hh Signaling Antagonist X, Itraconazole |
Buy |
| Sigma-Aldrich 1354251 | 100mg | $436 | Itraconazole United States Pharmacopeia (USP) Reference Standard |
Buy |
| TCI Chemical I0732 | 5g | $140 | Itraconazole >98.0%(HPLC)(T) |
Buy |
| TCI Chemical I0732 | 25g | $470 | Itraconazole >98.0%(HPLC)(T) |
Buy |
Itraconazole Chemical Properties,Usage,Production
Broad - spectrum antifungal agents
Itraconazole is an artificially synthetic clotrimazole, being a broad-spectrum synthetic antifungal agent. Its antimicrobial spectrum and antimicrobial mechanism is similar to clotrimazole, but has strong antibacterial activity against Aspergillus. It exerts its anti-fungal effect through changing the fungal cell membrane permeability with antibacterial activity against superficial and deep fungal pathogens. Its antibacterial spectrum is broader and stronger than ketoconazole, being able to inhibit the ergosterol synthesis of fungal cell membrane, thus playing the antifungal effect. This product is suitable for the treatment of Dermatophytes (Trichophyton, Microsporum, Flocculent Epidermophyton), Yeast [Cryptococcus neoformans, Pityrosporum, Candida (including Candida albicans, Candida glabrata and candida krusei)], Aspergillus, Histoplasma, Paracoccidioides brasiliensis, Sporothrix schenckii, Hormodendrum, Cladosporium, Blastomyces dermatitidis and various kinds of other types of yeasts and fungi. Itraconazole is not able to inhibit the growth of Rhizopus and Mucor.One nitrogen atom contained in the itraconazole molecule can bind to the ferrous ion on the heme of the P450 molecule in the fungal cell, thereby inhibiting the P450 hydroxylase-catalyzed de-methylation of lanosterol, Sterol to ergosterol conversion blocked, lanosterol and other precursors accumulation, membrane chemical composition changes, membrane associated enzyme dysfunction, increased permeability, intracellular fluid spill, so as to achieve the inhibition and sterilization. The combination of this product with the fungus P450 system is quite strong while its combination with the mammalian P450 system is weak, so that the toxicity of drugs on human is greatly reduced. Clinical Itraconazole is mainly used for the treatment of systemic deep fungal infections caused by systems such as blastomycosis, histoplasmosis, coccidioidomycosis, chromoblastomycosis, sporotrichosis and coccidioidomycosis. It can also be used for the treatment of candidiasis and aspergillosis.
The above information is compiled and edited by Tongtong from Chemicalbook.
Pharmacokinetics
Itraconazole, when taken immediately after the meal, can give the highest bioavailability. After (4.6 ± 1.3) hours of oral administration of 200 mg of itraconazole, the plasma concentration can reach peak with the plasma concentration being (0.32 ± 0.16) mg/mL. The product has a plasma protein binding rate of 99.8% with the whole blood concentration being about 60% of the plasma concentration. The drug concentration in the lung, kidney, liver, bone, stomach, spleen and muscle was found to be 2 to 3 times as high as that in the corresponding plasma concentration. In keratin-rich tissues, especially in the skin, the concentration is four times as high as that in the plasma concentration while the drug clearance is associated with the process of epidermal regeneration. If withdraw the drug after continuous medication of 4 weeks, the plasma concentration become undetectable after 7 days while drug contained in the skin can be still maintained in the drug treatment concentration for 2 to 4 weeks. After a week of starting the treatment, it can be measured of itraconazole in the keratin. At the end of the 3-month treatment course, the drug concentration can be maintained for at least 6 months. This product is present in sebum with a small amount also existing in sweat. Itraconazole is also concentrated in areas susceptible to fungal infection. The duration of the treatment concentration in the vaginal tissue is: 200mg once per day for 3 days, last for 2 days; 200mg 2 times a day for 1 day, can last 3 days. Itraconazole is mainly metabolized in the liver, producing large amounts of metabolites. One of them is hydroxylated itraconazole; in vitro study has found that it has a similar antifungal activity with this product. The level of antifungal drug measured by bioanalytical method is three times as high as the level measured by high-pressure liquid chromatography analysis. This product was biphasic in plasma clearance with the terminal half-life of (23.8 ± 4.7) hours. The dosage of the prototype drug through fecal excretion accounts for about 3 to 18% of the total dose. The prototype drug via renal excretion is less than 0.03% of the dose with about 35% being subject to urine excretion in the form of metabolites within a week.Clinical application and indications
Itraconazole is applicable for the treatment of the following diseases:1, it can be used for the treatment of systemic fungal infections, such as aspergillosis, candidiasis, cryptococcosis (including cryptococcal meningitis), histoplasmosis, sporotrichosis, Paracoccidioides brasiliensis disease, blastomycosis and many other kinds of rare systemic or tropical fungal diseases.
2, it can be used for the treatment of the candidiasis infection occurred in the mouth, throat (foreign data), esophageal (foreign data) and vulvovagina, and fungal conjunctivitis, fungal keratitis.
3, it can be used for the treatment of superficial fungal infections, such as hand, foot and ringworm, tinea corporis, tinea corporis, tinea versicolor and so on.
4, it can be used for the treatment of dermatophytes and (or) yeast-induced onychomycosis.
Dosage and Usage
Capsules: In order to achieve optimal absorption, itraconazole capsules should be administered immediately after a meal and the capsule must be swallowed. 1. Candida vaginitis: 200mg each time, twice a day, a course of treatment for 1 day or 200mg, once the course of treatment of 3 days; 2. Tinea versicolor: 200mg each time, once a day with the course of treatment of 7 days ; 3. Dermatomycosis: 100 mg each time, once a day with the course of treatment of 15 days; high-degree keratinized area (such as foot bottom ringworm, hand tinea) need: extended treatment of 15 days; 4 Oral candidiasis: 100mg each time, once a day with the course of treatment of 15 days; 5. Fungal keratitis: 200 mg each time, once a day with the course of treatment of 21 days; 6. For some immunodeficiency patients, such as leukemia (such as leukemia), AIDs and organ transplanted patients, application of itraconazole capsules for the treatment of fungal infections can get reduced oral bioavailability; in this case, the dose can be doubled. 7. Onychomycosis: 1) shock treatment: 200 mg each time, twice per day with continuous one week as a shock treatment. For the treatment of nail infections, it is recommended to adopt two shock treatment courses with each course having a gap of 3 weeks; for the treatment of toenail infection, it is recommended to adopt three shock treatment courses. Each treatment course has a gap of 3 weeks. 2) Or adopt continuous treatment: 200 mg each time, once a day, continue for three months. This product is removed more slowly in the skin and keratin tissue than removed in the plasma. Therefore, for skin infections, 2 to 4 weeks after stopping the drug can achieve the most ideal clinical and mycological efficacy. For the treatment of onychomycosis, people can achieve the best clinical and mycological efficacy after 6~9 months of stopping the drugs.Injection: during the first two days, give itraconazole injection 2 times a day, later change to once per day. Treatment protocol in Day 1 and 2: 2 times per day; adopt intravenous infusion of 200 mg itraconazole 1 hour each time. From day 3: perform once per day with intravenously infusion of 200 mg of itraconazole for 1 hour each time. The safety for intravenous administration of more than 14 days is not clear.
Medicine interactions
1. Enzyme-induction Drugs: for example, rifampicin and phenytoin can significantly reduce the oral bioavailability of this product. Therefore, upon administration together with the enzyme-induction drugs, we should monitor the plasma concentration of the goods.2 In vitro studies have showed that there was no interaction between itraconazole and imipramine, propranolol, diazepam, cimetidine, indomethacin, methotrexate and sulfadimidine regarding to the plasma protein binding.
3. It has been reported that this product, when exceeding the recommendation dosage, has interaction with cyclosporine A, astemizole and terfenadine. If these drugs are administrated together with this product, we should reduce their doses.
4. This product has been reported have interaction with warfarin and digoxin. Therefore, if these drugs are administrated together with this product, we should reduce their doses.
5. It has been not observed of the interaction of this product with AZT (zidovudine).
6. It has been not observed of the induction effects of itraconazole on the metabolism of ethinyl estradiol and norethindrone.
Adverse reactions
It is commonly observed of gastrointestinal discomfort, such as anorexia, nausea, abdominal pain and constipation. Less common side effects include headache, elevated reversible aminotransferase, menstrual disorders, dizziness and allergic reactions (such as itching, erythema, wheal and angioedema). There are a few cases that have reported Stevens-Johnson syndrome (severe erythema multiforme). The majority of patients who have had a potential pathologic change and are undergoing multiple drug regimens can get symptoms such as hypokalemia, edema, hepatitis, and alopecia during long-term treatment with itraconazole. There are individual cases that have reported the peripheral neuropathy, but whether it is related to taking itraconazole is uncertain.
Stability
This product appears as colorless to yellowish solution, should be stored at room temperature, being avoid of light and freezing. Before application, we should check whether there are particles emerging and whether there is discoloration. After the preparation of the solution, it can be stored for 48 h at room temperature or refrigerated and dark conditions.
Clinical evaluation
Tinea corporis, tinea corporis and tinea pedis can obtain the cure rate or significant efficiency of 80% or more. The cure rate of Pityriasis versicolor can be over 90%. The negative conversion ratio of vaginal candidiasis fungus can reach 80%. 80% of the cases of blastomycosis, sporotrichosis, and histoplasmosis can get clinically cured or markedly.Precautions
1. It is recommended to check liver function in patients who have continued medication for more than 1 month and who have develop anorexia, nausea, vomiting, fatigue, abdominal pain or dark urine during the treatment. If abnormal, they should stop medication.2. Itraconazole is mostly subject to the liver metabolism, and thus patients of abnormal liver function should take with caution (unless the need for treatment is higher than the risk of liver damage).
3. Stop the treatment immediately upon the occurrence of neurological symptoms.
4. For patients with renal insufficiency, the excretion of the goods slows down. It is recommended to monitor the plasma concentration of this product to determine the appropriate dose.
Drug overdose
Once occurs, we should take supportive therapy, including gastric lavage. Itraconazole can’t be removed by hemodialysis with no special antidote.Chemical properties
It is crystallized from toluene with the melting point of 166.2 °C and PKa of 3.7. It is almost insoluble in water and the dilute acid solution. Acute toxicity LD50 (14 days) mice, rats, dogs (mg/kg):> 320,> 320,> 200 orally.Uses
The imidazole antifungal agents for the triazole ring, through inhibiting the activation of cytochrome P-450, including oxidase and peroxidase, disable the 14, α-methyl sterols to be dehydrogenated and be converted to ergosterol, so that the growth and proliferation of fungi are inhibited. They have strong lipophilicity and penetrate through the biofilm to inhibit the binding of the membrane to the fungus. The antibacterial spectrum is similar to ketoconazole. It is effective in the treatment of superficial fungal diseases such as vaginal and oral candidiasis as well as skin mycosis. Furthermore, it is expected to become the highly-efficient and safe drugs for the treatment of deep fungal infections such as cryptococcal encephalitis (AIDS). It is used for the treatment of vulvovaginal candidiasis, pityriasis and skin fungal disease pityriasis caused by sensitive fungi.It can be used for the synthesis of broad-spectrum azole antifungal agents for the treatment of systemic infection caused by deep fungus. It can also be used for the treatment of candidiasis and aspergillosis.
Production method
Starting from m-dichlorobenzene, compound (I) can be obtained through a reaction similar to ketoconazole. The compound (I) is further condensed with 1-acetyl-4-(4-hydroxyphenyl) piperazine, followed by hydrolysis to remove the acetyl group, condensation with p-nitrochlorobenzene, hydrogenation reduction, chloroformate esterification, and reaction with hydrazine hydrate. After cyclization and alkylation, itraconazole is finally obtained. The intermediate 1-acetyl-4-(4-hydroxyphenyl) piperazine can use piperazine as the starting material and prepared with the following reactions.Description
Itraconazole is an orally-active triazole antifungal indicated for use in the treatment of dermal, vaginal and systemic mycoses. In immunocompromised and AIDS patients, itraconazole has been shown to significantly reduce the incidence of relapses of cryptococcal meningitis.Chemical Properties
Off-White Crystalline SolidOriginator
Janssen (Belgium)Uses
A traizole antifungal agentUses
For the treatment of the following fungal infections in immunocompromised and non-immunocompromised patients: pulmonary and extrapulmonary blastomycosis, histoplasmosis, aspergillosis, and onychomycosis.Uses
vitamin, enzyme cofactorUses
Anti-infectiveUses
An orally active antimycotic structurally related to Ketoconazole. AntifungalUses
Anti Fungal. Used in the treatment of stomach upset/ indigestion and other gastrointestinal conditionsUses
Itraconazole is a triazole antifungal agent. It is used to inhibit cytochrome P-450-dependent enzymes and ergosterol synthesis. It has been used against histoplasmosis, blastomycosis, cryptococcal meningitis, and aspergillosis. It?s different formulations are used to study Candida strains in murine invasive infections. It has been used to study proliferative changes of the forestomach mucosa in alloxan-induced diabetic rats..Indications
Itraconazole (Sporanox) is effective in the treatment of histoplasmosis, blastomycosis, candidiasis, and dermatophyte infection. Its efficacy in the treatment of tinea capitis in children is equal to griseofulvin, and it is usually better tolerated (21). It is metabolized by the cytochrome P-450 system and may increase the levels ofwarfarin, cyclosporine, and digoxin among others. Its use is contraindicated with certain medications.Itraconazole (Sporanox) is a triazole antifungal that is related to the imidazole ketoconazole. Similar to ketoconazole, it interferes with ergosterol synthesis and cell membrane integrity. It is clinically active against dimorphic fungi, yeast, dermatophytes, Blastomycetes, histoplasmosis, sporotrichosis, and Aspergillus. Itraconazole is a potent inhibitor of the cytochrome P450 3A enzyme system, which may elevate blood levels of other drugs metabolized by this system if taken concomitantly. Itraconazole levels may decrease in patients who are concurrently taking rifampin, phenobarbital, or phenytoin. Cyclosporine, felodipine, digoxin, warfarin, and oral hypoglycemic levels may increase when given in conjunction with itraconazole. Itraconazole, like ketoconazole, is contraindicated in patients taking cisapride. Itraconazole may induce torsades de pointes, ventricular arrhythmias, and congestive heart failure.
Definition
ChEBI: Itraconazole is an N-arylpiperazine that is cis-ketoconazole in which the imidazol-1-yl group is replaced by a 1,2,4-triazol-1-yl group and in which the actyl group attached to the piperazine moiety is replaced by a p-[(+-)1-sec-butyl-5-oxo-1,5-dihydro-4H-1,2,4-triazol-4-yl]phenyl group. A potent P-glycoprotein and CYP3A4 inhibitor, it is used as an antifungal drug for the treatment of various fungal infections, including aspergillosis, blastomycosis, candidiasis, chromoblastomycosis, coccidioidomycosis, cryptococcosis, histoplasmosis, and sporotrichosis. It has a role as a P450 inhibitor, an EC 3.6.3.44 (xenobiotic-transporting ATPase) inhibitor and a Hedgehog signaling pathway inhibitor. It is a member of triazoles, a dioxolane, a N-arylpiperazine, a dichlorobenzene, a cyclic ketal, a conazole antifungal drug, a triazole antifungal drug and an aromatic ether.Manufacturing Process
Synthesis of cis-4-{4-[4-{4-[2-(2,4-dichlorophenyl)-2-(1H-1,2,4-triazol-1- ylmethyl)-1,3-dioxolan-4-ylmethoxy]phenyl}-1-piperazinyl]phenyl}-2,4- dihydro-2-(methylpropyl)-3H-1,2,4-triazol-3-one is showed by the same procedure as for cis-4-{4-[4-{4-[2-(2,4-dichlorophenyl)-2-(1H-1,2,4-triazol-1- ylmethyl)-1,3- dioxolan-4-ylmethoxy]phenyl}-1-piperazinyl]phenyl}-2,4-dihydro-2-propyl-3H-1,2,4-triazol-3-one described in the patent.A mixture of 13.4 parts of 1-(4-methoxyphenyl)piperazine dihydrochloride, 7.9 parts of 1-chloro-4-nitrobenzene, 10 parts of potassium carbonate and 90 parts of N,N-dimethylformamide is stirred and refluxed overnight. The reaction mixture is diluted with water and the product is extracted twice with trichloromethane. The residue is triturated in 4-methyl-2-pentanone. The product is filtered off and crystallized from 1,4-dioxane, yielding 10.5 parts (67%) of 1-(4-methoxyphenyl)-4-(4-nitrophenyl)piperazine; melting point 195.1°C.
A mixture of 12 parts of 1-(4-methoxyphenyl)-4-(4-nitrophenyl)piperazine, 200 parts of methanol and 225 parts of tetrahydrofuran is hydrogenated at normal pressure and at 20°C with 2 parts of palladium-on-charcoal catalyst 10%. After the calculated amount of hydrogen is taken up, the catalyst is filtered off and washed with N,N-dimethylacetamide. Product is filtered off and crystallized from 1-butanol, yielding 8 parts (74%) of 4-[4-(4- methoxyphenyl)-1-piperazinyl]benzenamine; melting point 191.8°C.
A mixture of 30 parts of 4-[4-(4-methoxyphenyl)-1-piperazinyl]benzenamine and 300 parts of a hydrobromic acid solution 48% in water is stirred and refluxed for 10 days. The reaction mixture is evaporated and the residue is alkalized with sodium hydroxide. The mixture is filtered and the filtrate is acidified with acetic acid. The precipitated product is filtered off and crystallized from 1,4-dioxane, yielding 12 parts (44%) of 2,4-dihydro-4-{4-[4- (4-hydroxyphenyl)-1-piperazinyl]phenyl}-2-(1-methylpropyl)-3H-1,2,4-triazol- 3-one.
To a stirred solution of 2,4-dihydro-4-{4-[4-(4-hydroxyphenyl)-1-piperazinyl] phenyl}-2-(1-methylpropyl)-3H-1,2,4-triazol-3-one in 100 parts of dimethyl sulfoxide are added 0.3 parts of sodium hydride dispersion 78% and the whole is stirred at 50°C till foaming has ceased. Then there are added 3.7 parts of cis-[2-(2,4-dichlorophenyl)-2-(1H-1,2,4-triazol-1-ylmethyl)-1,3- dioxolan-4-ylmethyl]methanesulfonate and stirring is continued for 3 hours at 100°C. The reaction mixture is cooled and poured onto water. The product is extracted with dichloromethane. The extracts are washed with a diluted sodium hydroxide solution and filtered. The residue is crystallized from 1- butanol. The product yield 4.3 parts (75%) of cis-4-{4-[4-{4-[2-(2,4- dichlorophenyl)-2-(1H-1,2,4-triazol-1-ylmethyl)-1,3-dioxolan-4-ylmethoxy] phenyl}-1-piperazinyl]phenyl}-2,4-dihydro-2-(methylpropyl)-3H-1,2,4-triazol- 3-one.
brand name
Sporanox (Janssen).Therapeutic Function
AntifungalAntimicrobial activity
The spectrum includes dermatophytes, dimorphic fungi (Blast. dermatitidis, Coccidioides spp., Hist. capsulatum, Paracocc. brasiliensis, Penicillium marneffei and Spor. schenckii), molds (including Aspergillus spp.), dematiaceous fungi and yeasts (Candida spp. and Cryptococcus spp.).Acquired resistance
This is uncommon, but fluconazole-resistant C. albicans and C. glabrata are often cross-resistant to itraconazole. There are reports of itraconazole-resistant strains of A. fumigatus.General Description
Itraconazole is an antifungal drug prescribed for oral or intravenous treatment of fungal infections. The drug is sold under trade names such as Sporanoxor Onmel?. This Certified Spiking Solution? is suitable as starting material for calibrators, controls, or linearity standards for clinical and diagnostic testing or therapeutic drug monitoring of itraconazole in patient blood, serum, or plasma samples by LC-MS/MS or HPLC.Pharmaceutical Applications
A synthetic dioxolane triazole available for oral or parenteral administration.Biochem/physiol Actions
Itraconazole inhibits cytochrome P-450-dependent enzymes which results in the inhibition of ergosterol synthesis. It does so by interacting with 14-α demethylase, which is a cytochrome P-450 enzyme necessary to convert lanosterol to ergosterol. Ergosterol is a crucial compenent of fungal cell membranes. Therefore, it′s inhibition results in increased cellular permeability causing leakage of cellular contents. Itraconazole may also inhibit endogenous respiration, interact with membrane phospholipids, inhibit the transformation of yeasts to mycelial forms, inhibit purine uptake, and impair triglyceride and phospholipid biosynthesis.Pharmacokinetics
Oral absorption: 30% (capsules); 55% (solution)Cmax 100 mg oral: 0.1–0.2 mg/L after 2–4 h
Plasma half-life: 20–30 h
Volume of distribution: 11 L/kg
Plasma protein binding: >99%
Absorption
Absorption is improved if the drug is given with food or an acidic beverage. In contrast, absorption is reduced if it is given together with compounds that reduce gastric acid secretion. Higher concentrations are obtained with repeated dosing, but there is much individual variation. Incorporation into a solution of hydroxypropyl-β-cyclodextrin enhances bioavailability and leads to much higher blood levels in neutropenic individuals and persons with AIDS. This formulation is better absorbed if given without food. Increases in dosage produce disproportionate changes in blood concentrations.
Distribution
Levels in the CSF are low, but concentrations in lung, liver and bone are 2–3 times higher than in serum, and concentrations in the genital tract are 3–10 times higher. High concentrations are also found in the stratum corneum, as a result of drug secretion in sebum. The drug persists in the skin and nails for weeks to months after treatment is discontinued.
Metabolism and excretion
It is degraded by the liver into a large number of (mostly inactive) metabolites which are excreted with the bile and urine. Itraconazole is unusual because the major metabolite, hydroxyitraconazole, is bioactive and has a similar spectrum of activity as the parent compound. In the steady state, this metabolite is found at serum concentrations about two-fold higher than those of the parent drug. About 80–90% of the intravenous carrier, hydroxypropyl-β-cyclodextrin, is excreted unchanged in the urine. No adjustment of dosage is required in hepatic or renal failure, or during hemodialysis or peritoneal dialysis.
Clinical Use
AspergillosisSystemic mycoses with dimorphic fungi (blastomycosis, coccidioidomycosis, histoplasmosis, paracoccidioidomycosis, penicilliosis) Subcutaneous mycoses (chromoblastomycosis, sporotrichosis)
Mucosal and cutaneous candidosis.
Dermatophytosis
Phaeohyphomycosis
Pityriasis versicolor
Side effects
Unwanted effects are more common with oral solution than with capsules, and are more severe. They include nausea, abdominal discomfort, dyspepsia, diarrhea, headache, pruritus and skin rash. Rare side effects include Stevens–Johnson syndrome, transient abnormalities of liver enzymes, reversible idiosyncratic hepatitis and hypokalemia.Intravenous itraconazole has been associated with congestive heart failure. Neither intravenous nor oral itraconazole should be used to treat infections in patients with evidence of ventricular dysfunction unless the expected benefit clearly exceeds the risk. Patients with risk factors for congestive heart failure should be treated with caution and their condition monitored.
Veterinary Drugs and Treatments
Itraconazole may have use in veterinary medicine in the treatment of systemic mycoses, including aspergillosis, cryptococcal meningitis, blastomycosis, and histoplasmosis. Itraconazole is probably more effective than ketoconazole, but is significantly more expensive. It may also be useful for superficial candidiasis or dermatophytosis,Itraconazole does not have appreciable effects (unlike ketoconazole) on hormone synthesis and may have fewer side effects than ketoconazole in small animals.It is considered by many to be the drug of choice for treating blastomycosis, unless moderate or severe hypoxemia is present (than amphotericin B).
In horses, itraconazole may be useful in the treatment of sporotrichosis and Coccidioides immitis osteomyelitis.
in vitro
itraconazole was metabolized into hydroxy-itraconazole (oh-itz), a known in vivo metabolite of itz, and two new metabolites: keto-itraconazole (keto-itz) and n-desalkyl-itraconazole (nd-itz). itraconazole was a substrate for cyp3a and to characterize the metabolites generated. itraconazole exhibited an unbound km of 3.9 nm for cyp3a. itraconazole metabolites are as potent as or more potent cyp3a4 inhibitors than itz itself [1]. itraconazole was pharmacologically distinct from other azole antifungal agents. itraconazole has been shown to inhibit both the hedgehog signaling pathway and angiogenesis [2] itraconazole was active against 60 clinical isolates of aspergillus spp. with geometric mean (gm) mics of 0.25 mg/ml [3]. itraconazoleshowed an affinity for mammalian cytochrome p-450 enzymes as well as for fungal p-450-dependent enzyme, and thus has the potential for clinically important interactions [4].in vivo
oral administration of itraconazole (200 mg) once daily for 4 days increased the area under the midazolam concentration-time curve from 10 to 15 times (p < 0.001) and mean peak concentrations three to four times (p < 0.001) compared with the placebo phase [5].storage
Store at -20°CReferences
1) Vanden Bossche?et al.?(1993),?Effects of itraconazole on cytochrome P-450-dependent sterol 14 alpha-demethylation and reduction of 3-ketosteroids in Cryptococcus neoformans; Antimicrob. Agents Chemother.,?37?2101 2) Liu?et al.?(2014),?Itraconazole suppresses the growth of glioblastoma through induction of autophagy: involvement of abnormal cholesterol trafficking; Autophagy,?10?1241 3) Kim?et al. (2010),?Itraconazole, a commonly used antifungal that inhibits Hedgehog pathway activity and cancer growth; Cancer Cell,?17?388 4) Nacev?et al. (2011),?The antifungal drug itraconazole inhibits vascular endothelial growth factor receptor 2 (VEGFR2) glycosylation, trafficking, and signaling in endothelial cells; J. Biol. Chem.,?286?44045Preparation Products And Raw materials
Itraconazole Supplier
| Supplier | Tel | Country | ProdList | Advantage | |
|---|---|---|---|---|---|
| +8613288715578 | sales@hbmojin.com | China | 12453 | 58 | |
| +8617531190177 | peter@yan-xi.com | China | 5993 | 58 | |
| +86-13176845580 +86-13176845580 |
da@zhongda-biotech.com | China | 248 | 58 | |
| +8619956560829 | justine@zhongda-biotech.com | China | 300 | 58 | |
| +8615689548120 | linda@zhongda-biotech.com | China | 204 | 58 | |
| +8617756083858 | daisy@anhuiruihan.com | China | 994 | 58 | |
| +undefined15081010295 | 2691956269@qq.com | China | 359 | 58 | |
| +undefined86-15315557071 | sales02@airuikechemical.com | China | 994 | 58 | |
| +86-13474506593 +86-13474506593 |
sarah@tnjone.com | China | 848 | 58 | |
| 571-85586718 +8613336195806 |
sales@capotchem.com | China | 29797 | 60 |
Related articles
What is itraconazole used to treat?
Itraconazole is a triazole antimycotic itraconazole used to treat systemic infections such as candidosis and aspergillosis including disseminated infections, blastomycosis, coccidioidomycosis, histoplasmosis, and cryptococcosis.
Mar 16,2024
Itraconazole (Sporanoxs) is a synthetic triazole drug developed in the 1980s as the first orally bioavailable triazole agent. Similar to posaconazole, it contains a piperazine-phenyl-triazole side chain.
Mar 28,2022
Itraconazole Spectrum
84625-61-6, ItraconazoleRelated Search
- Cis-2-(2,4-DichloroPhenyl)-2(Ih-I,2,4-Triazol-L-Yl-Methy>>-L,3-Dioxolan-4-MethanolMethaneSulfonate,Itraconazole,
- 1,4-Dioxane
- DIOXOPROMETHAZINE HCL
- HYDROXY ITRACONAZOLE
- Dichloromethylphenylsilane
- Dichlorodiphenylsilane
- Selenium dioxide
- 8-[(E)-2-(3,4-dimethoxyphenyl)ethenyl]-1,3-diethyl-7-methyl-purine-2,6 -dione
- Ipamorelin
- 1-(4-chlorophenyl)-4-morpholin-4-yl-5H-imidazol-2-one
1of4
The What'sApp is temporarily not supported in mainland China